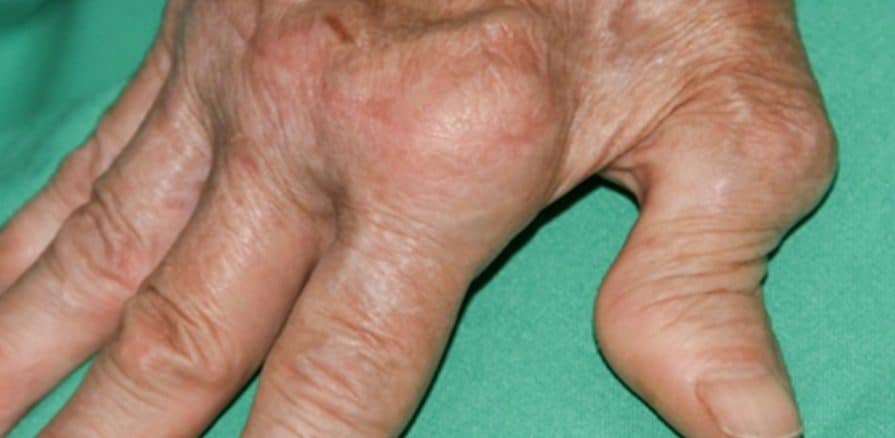
Rheumatoid arthritis (RA) is a chronic inflammatory disorder that primarily targets the joints but can affect various body systems. Unlike osteoarthritis (OA), which results from cartilage wear and tear over time, RA’s exact cause remains unknown. It is likely that genetic and environmental factors contribute to the onset of RA.
Risk Factors for Rheumatoid Arthritis (RA)
Susceptibility Factors
- Age: RA risk increases with age, plateauing around 50.
- Sex: Women are three times more likely to develop RA than men.
- Genetics: A family history of RA increases the likelihood of developing the condition.
Initiating Factors
- Infections: Alterations in gut or mouth bacteria may trigger RA. Periodontitis is a notable risk factor.
- Smoking: A well-known risk factor for RA.
- Stress: Emotional stress or trauma often precedes the onset of RA.
Symptoms of Rheumatoid Arthritis (RA)
General Symptoms
- Fatigue
- Muscle pain
- Low-grade fever
- Weight loss
- Numbness or tingling in the hands
Joint Symptoms
- Pattern: RA typically affects the same joints on both sides of the body.
- Affected Joints: Commonly involves the hands, wrists, elbows, shoulders, feet, ankles, knees, hips, neck, and cricoarytenoid joint.
- Stiffness: Notable in the morning and after periods of inactivity, often lasting over an hour.
Other Symptoms
- Bone loss
- Muscle weakness
- Skin nodules
- Eye inflammation
- Lung disease
- Pericarditis
- Vasculitis
- Sjögren’s syndrome
- Fatigue
- Amplified pain
- Heart disease
- Increased cancer risk
Diagnosis of Rheumatoid Arthritis (RA)
Diagnosing RA involves identifying signs of inflammation in three or more joints for six weeks or longer. Key diagnostic indicators include:
- Positive diagnostic antibody blood tests (rheumatoid factor or anti-citrullinated peptide/protein antibody)
- Elevated C-reactive protein or erythrocyte sedimentation rate
Treatment of Rheumatoid Arthritis (RA)
The primary goals of RA treatment are to control symptoms, minimize joint damage, and improve quality of life through a combination of medications and non-drug therapies.
General Principles
- Early treatment initiation is crucial.
- Regular medical care and monitoring for side effects are necessary.
Non-Pharmacologic Therapies
- Education and Counseling: Helps patients understand RA and develop coping strategies.
- Exercise: Range-of-motion, strength-building, and endurance activities are beneficial.
- Physical and Occupational Therapy: Focus on functional training, balance training, and the use of splints, braces, orthotics, and assistive devices.
- Nutrition: A Mediterranean diet, along with supplements such as folic acid, omega-3, and vitamin D3, supports nutrition and weight management.
- Smoking and Alcohol: It is important to quit smoking and consume alcohol with caution.
- Bone Loss Measures: Include adequate calcium and vitamin D intake, minimizing steroid use, and maintaining physical activity.
Medications
- DMARDs: Such as Methotrexate, are commonly prescribed.
- NSAIDs: Help with pain relief and minor inflammation reduction.
- Steroids and Pain Medications: Manage severe symptoms and side effects.
Disease Course and Management
RA progression varies widely among individuals. While untreated RA often leads to progressive joint damage and disability, early and consistent treatment can reduce symptoms, slow disease progression, and improve quality of life. Most people require lifelong treatment, but remission is possible, though rare without medication. Regular follow-ups with a rheumatologist are essential to tailor treatment plans, manage symptoms, and monitor for potential complications.